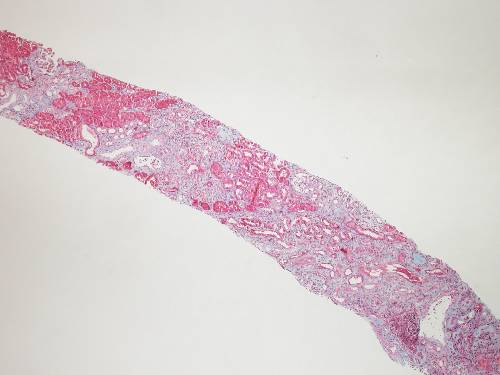
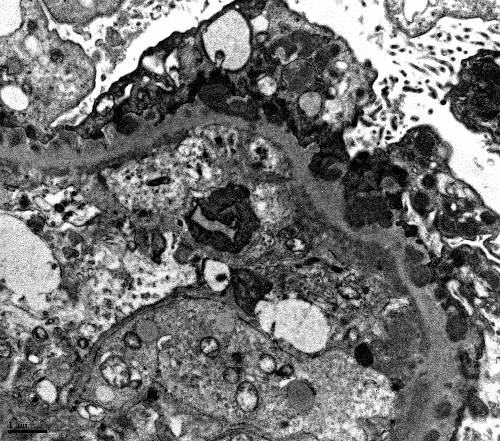
A 40 year-old pleasant African man with ESRD secondary to FSGS started automated peritoneal dialysis. His prescription includes 2.5 L and 3 exchanges over 8 hours at night with a last fill of 2 L. He has a urine output of 1000 mL/day. A typical ultrafiltration on cycler is used at 1000 mL. Average drain volume of the day dwell was 1500 mL prior to going on the cycler at night.
He came with complains of lower abdominal wall edema extending to the scrotum over the past 5 days. Without any change in the dialysis prescription, his drain volume before going on the cycler dropped to 900 mL, and the ultrafiltration volume on the cycler came down to 100 mL. He reports no pain with fill or drain.
What is the next step?
| A. Chest X ray PA and lateral view | |
| B. Drain the fluid middle of the day to reduce the dwell time | |
|
|
C. PD catheter manipulation |
|
|
D. Abdominal CT scan with contrast in the dialysate |
| E. Switch to hemodialysis | |
| F. Pleurodesis |
|
|
Copyright © ABIM Exam World
Created On: 09/14/2017
Last Modified: 08/06/2018